Knee Arthritis
Osteoarthritis is a common condition affecting more than 10 million people in the UK. It is a disease process in which the joint surface wears away resulting in underlying bone becoming exposed. During weightbearing activities the exposed bones rub against each other causing pain, swelling and inflammation.
Often there is no obvious cause for the development of arthritis but some associated risk factors are:
- Previous injuries such as ligament tears or fractures
- Body weight
- Previous removal of meniscal cartilage
- Genetic factors
- Alignment of the limb
- Inflammatory arthritis
Symptoms
Generally, symptoms begin in patients over the age of 50 and the incidence increases with age. It can occur in younger patients as a result of trauma or other childhood injuries.
Common symptoms are:
- Pain – worse after exercise, often causes disturbed sleep
- Stiffness – worse in the morning or after having been seated for a time
- Swelling – Intermittent episodes of joint swelling often accompanied by a flare up of pain
- Instability – the knee can give way, sometimes due to pain but also if the collateral ligaments become incompetent
The symptoms will deteriorate with time and often the symptoms can fluctuate with time and the weather.
Treatments
Non-operative
In the early stages of arthritis the majority of people can be managed without surgery.
Treatment involves:
- Optimizing pain killer medication often using anti-inflammatories
- Reducing weight and so reducing the forces the joint has to withstand
- Stopping strenuous exercises or work
- Using a stick, crutch or knee brace
- Maintaining movement and increasing muscle strength with physio directed exercises.
- Joint injections using steroid and local anaesthetic or hyaluronic acid
With time, as the joint becomes more worn out or non-operative treatment fails, joint replacement surgery is recommended.
Operative
Partial Knee Replacement
Often only one compartment (medial, lateral, patella) of the knee wears out and the remaining cartilage and ligaments in the other compartments are preserved and in a good condition. In this situation a partial (unicompartmental) knee replacement is indicated.
A partial knee replacement:
- Preserves ligaments within the knee – this confers better functional results following surgery
- Preserves bone for any future surgery
- Less traumatic - allows for a quicker recovery and reduced inpatient admission

Through a minimally invasive incision the inner compartment of the knee is replaced with a mobile bearing prosthesis. This consists of a metal femoral and tibial component with a polyethelene (plastic) insert that moves as the knee bends. The cruciate ligaments are preserved so the knee will feel ‘more normal’ thus providing improved functional results following surgery.
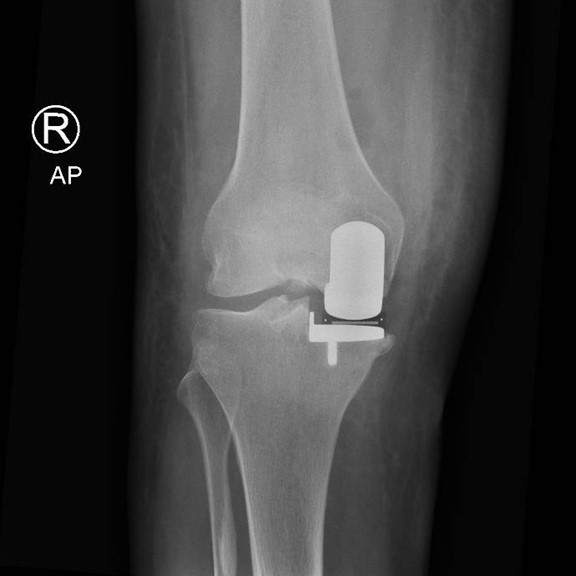
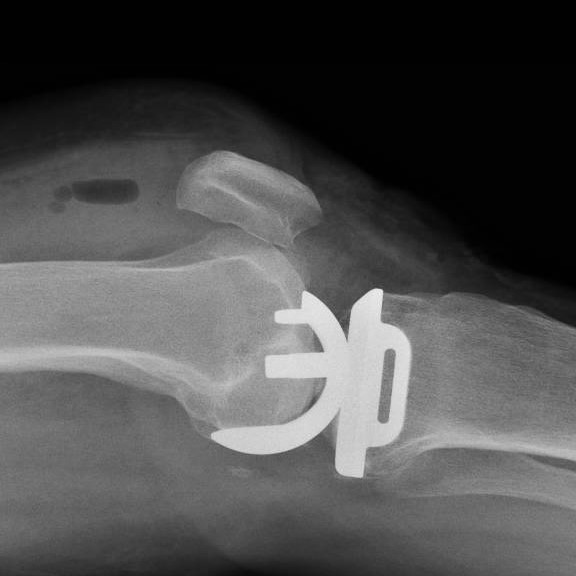
You will be admitted on the day of surgery having not eaten for the preceding 6 hours prior to the operation (nil by mouth). The anaesthetist will talk to you regarding the type of anaesthetic (spinal or general anaesthetic), it is preferable to have a spinal anaesthetic as there are fewer side effects, improved pain control and a speedier rehabilitation whilst in hospital. See FAQ section spinal or general anaesthetic.
After surgery, patients generally remain inpatients for 1-3 days. Patients mobilise full weight bearing on the same day of their surgery and generally go home using a stick or crutch for 1-2 weeks. After 4-6 weeks the vast majority of patients will have seen a significant improvement in their knee function.
Risks of surgery
Common
- Bleeding – Bruising following the surgery is common, very occasionally a blood transfusion or iron tablets may be required. Rarely, the bleeding may form a collection within the knee joint which may require a further operation to remove it.
- Blood Clots – Deep vein thrombosis (DVT) is a blood clot in a vein. The risk of developing a DVT is greater after surgery (especially lower limb surgery). A DVT can pass in the blood stream and become lodged in the lungs causing a pulmonary embolus (see below). To limit the risk of DVTs forming you will be given stockings to wear on your legs whilst an inpatient and a daily tablet or injection to thin the blood. Moving early after surgery is one of the best ways to prevent blood clots from forming.
- Pain – The knee will be sore after the operation. Pain will improve with time and generally is much improved by the 2 week post-operative mark. Rarely, pain can be a chronic problem.
- Knee Stiffness – This may occur after the operation, especially if the knee is stiff before surgery. If this continues for some time, despite physio input, a manipulation under anaesthesia may be recommended.
- Implant wear and loosening – With modern operating techniques and new implants, knee replacements last in excess of 20 years. In some cases, they can fail and this is often as a result of the plastic liner wearing out.
- Progression of arthritis – Arthritis can progress into the other compartments of the knee with time. This can eventually lead to pain and need for further surgery.
Less Common
- Infection – You will receive antibiotics just before the operation starts and the procedure is performed in a sterile theatre. The wound site may become red, hot and painful. There may be a discharge of pus or fluid. This is usually treated with antibiotics and an operation to washout the joint may be necessary. In rare cases, the implant may be removed and replaced at a later date (revision surgery). The infection can sometimes lead to sepsis (blood infection) and strong antibiotics are required.
Rare
- Pulmonary Embolism – This happens when a blood clot (DVT) breaks off and lodges within the lungs. It can affect breathing and is a serious condition that can be fatal.
- Poor scars – The wound may become red, thickened and painful (keloid scar); this is more common in Afro-Caribbeans.
- Nerve Injuries – Efforts are made to prevent this, however damage to the small nerves of the knee is a risk. This may cause temporary or permanent altered sensation or movement around the knee and lower leg. It is common to have a patch of numbness to the outer aspect of the knee, this generally resolves with time.
- Fracture – Bone may be broken when the new implant is inserted. This may require fixing immediately or at a later date.
- Instability – Rarely the reconstructed joint can be unstable and this can require further surgery.
- Blood vessel injury – Blood vessels at the back of the knee may be damaged, this can require further surgery by the vascular surgeons.
- Meniscal bearing dislocation – the mobile plastic insert can be displaced out of the joint. This causes pain and knee dysfunction requiring revision surgery.

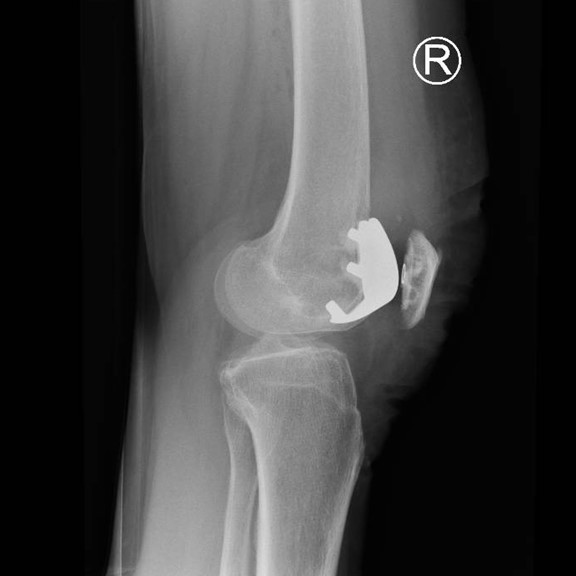
Through a minimally invasive midline incision the patellofemoral joint of the knee is replaced. This consists of a metal femoral component and a polyethelene (plastic) patella button. The unaffected medial and lateral parts of the joint are preserved along with the cruciate ligaments so the knee will feel ‘more normal’ thus providing improved functional results following surgery.
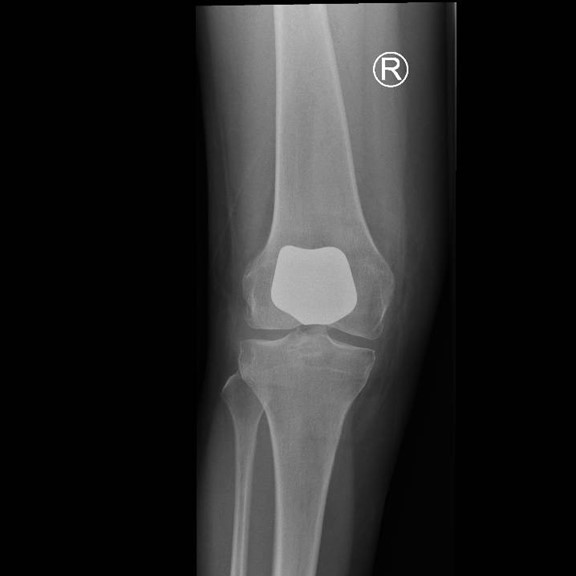
You will be admitted on the day of surgery having not eaten for the preceding 6 hours prior to the operation (nil by mouth). The anaesthetist will talk to you regarding the type of anaesthetic (spinal or general anaesthetic), it is preferable to have a spinal anaesthetic as there are fewer side effects, improved pain control and a speedier rehabilitation whilst in hospital. See FAQ section spinal or general anaesthetic.
After surgery patients generally remain inpatients for 1-3 days. Patients mobilise full weight bearing on the same day of their surgery and generally go home with a stick or crutch for 1-2 weeks. After 4-6 weeks the vast majority of patients will have seen a significant improvement in their knee function.
Risks of surgery
Common
- Bleeding – Bruising following the surgery is common, very occasionally a blood transfusion or iron tablets may be required. Rarely, the bleeding may form a collection within the knee joint which may require a further operation to remove it.
- Blood Clots – Deep vein thrombosis (DVT) is a blood clot in a vein. The risk of developing a DVT is greater after surgery (especially lower limb surgery). A DVT can pass in the blood stream and become lodged in the lungs causing a pulmonary embolus (see below). To limit the risk of DVTs forming you will be given stockings to wear on your legs whilst an inpatient and a daily tablet or injection to thin the blood. Moving early after surgery is one of the best ways to prevent blood clots from forming.
- Pain – The knee will be sore after the operation. Pain will improve with time and generally is much improved by the 2 week post-operative mark. Rarely, pain can be a chronic problem.
- Knee Stiffness – This may occur after the operation, especially if the knee is stiff before surgery. If this continues for some time, despite physio input, a manipulation under anaesthesia may be recommended.
- Implant wear and loosening – With modern operating techniques and new implants, knee replacements last in excess of 20 years. In some cases they can fail and this is often as a result of the plastic liner wearing out.
- Progression of arthritis – Arthritis can progress into the other compartments of the knee with time. This can eventually lead to pain and need for further surgery
Less Common
- Infection – You will receive antibiotics just before the operation starts and the procedure is performed in a sterile theatre. The wound site may become red, hot and painful. There may be a discharge of pus or fluid. This is usually treated with antibiotics and an operation to washout the joint may be necessary. In rare cases, the implant may be removed and replaced at a later date (revision surgery). The infection can sometimes lead to sepsis (blood infection) and strong antibiotics are required.
Rare
- Pulmonary Embolism – This happens when a blood clot (DVT) breaks off and lodges within the lungs. It can affect breathing and is a serious condition that can be fatal.
- Poor scars – The wound may become red, thickened and painful (keloid scar); this is more common in Afro-Caribbeans.
- Nerve Injuries – Efforts are made to prevent this, however damage to the small nerves of the knee is a risk. This may cause temporary or permanent altered sensation or movement around the knee and lower leg. It is common to have a patch of numbness to the outer aspect of the knee, this generally resolves with time.
- Fracture – Bone may be broken when the new implant is inserted. This may require fixing immediately or at a later date.
- Instability – Rarely the reconstructed joint can be unstable and this can require further surgery.
- Blood vessel injury – Blood vessels at the back of the knee may be damaged, this can require further surgery by the vascular surgeons.
It is rare to have isolated lateral (outer) compartment arthritis. Through a minimally invasive incision the outer compartment of the knee is replaced with a fixed bearing prosthesis. This consists of a metal femoral and tibial component with a polyethelene (plastic) insert that is fixed to the tibial component.

You will be admitted on the day of surgery having not eaten for the preceding 6 hours prior to the operation (nil by mouth). The anaesthetist will talk to you regarding the type of anaesthetic (spinal or general anaesthetic), it is preferable to have a spinal anaesthetic as there are fewer side effects, improved pain control and a speedier rehabilitation whilst in hospital. See FAQ section spinal or general anaesthetic.
After surgery patients generally remain inpatients for 1-3 days. Patients mobilise full weight bearing on the same day of their surgery and generally go home with a stick or crutch for 1-2 weeks. After 4-6 weeks the vast majority of patients will have seen a significant improvement in their knee function.
Risks of surgery
Common
- Bleeding – Bruising following the surgery is common, very occasionally a blood transfusion or iron tablets may be required. Rarely, the bleeding may form a collection within the knee joint which may require a further operation to remove it
- Blood Clots – Deep vein thrombosis (DVT) is a blood clot in a vein. The risk of developing a DVT is greater after surgery (especially lower limb surgery). A DVT can pass in the blood stream and become lodged in the lungs causing a pulmonary embolus (see below). To limit the risk of DVTs forming you will be given stockings to wear on your legs whilst an inpatient and a daily tablet or injection to thin the blood. Moving early after surgery is one of the best ways to prevent blood clots from forming.
- Pain – The knee will be sore after the operation. Pain will improve with time and generally is much improved by the 2 week post-operative mark. Rarely, pain can be a chronic problem.
- Knee Stiffness – This may occur after the operation, especially if the knee is stiff before surgery. If this continues for some time, despite physio input, a manipulation under anaesthesia may be recommended.
- Implant wear and loosening – With modern operating techniques and new implants, knee replacements last in excess of 20 years. In some cases they can fail and this is often as a result of the plastic liner wearing out.
- Progression of arthritis – Arthritis can progress into the other compartments of the knee with time. This can eventually lead to pain and need for further surgery.
Less Common
- Infection – You will receive antibiotics just before the operation starts and the procedure is performed in a sterile theatre. The wound site may become red, hot and painful. There may be a discharge of pus or fluid. This is usually treated with antibiotics and an operation to washout the joint may be necessary. In rare cases, the implant may be removed and replaced at a later date (revision surgery). The infection can sometimes lead to sepsis (blood infection) and strong antibiotics are required.
Rare
- Pulmonary Embolism – This happens when a blood clot (DVT) breaks off and lodges within the lungs. It can affect breathing and is a serious condition that can be fatal.
- Poor scars – The wound may become red, thickened and painful (keloid scar); this is more common in Afro-Caribbeans.
- Nerve Injuries – Efforts are made to prevent this, however damage to the small nerves of the knee is a risk. This may cause temporary or permanent altered sensation or movement around the knee and lower leg. It is common to have a patch of numbness to the outer aspect of the knee, this generally resolves with time.
- Fracture – Bone may be broken when the new implant is inserted. This may require fixing immediately or at a later date.
- Instability – Rarely the reconstructed joint can be unstable and this can require further surgery.
- Blood vessel injury – Blood vessels at the back of the knee may be damaged, this can require further surgery by the vascular surgeons.
Total Knee Replacement
When more than one compartment (medial, lateral, patella) of the knee wears out and non-operative treatment options have failed a total knee replacement is required.
Procedures:
If the arthritis within the knee affects more than one compartment then a total knee replacement may be recommended.
In a conventional knee replacement, instruments are used to perform the bony cuts and restore the knee back to its original (mechanical) position. This involves releasing some of the ligaments and soft tissues around the knee so that a balanced, full range of motion is achieved at the end of the surgery.


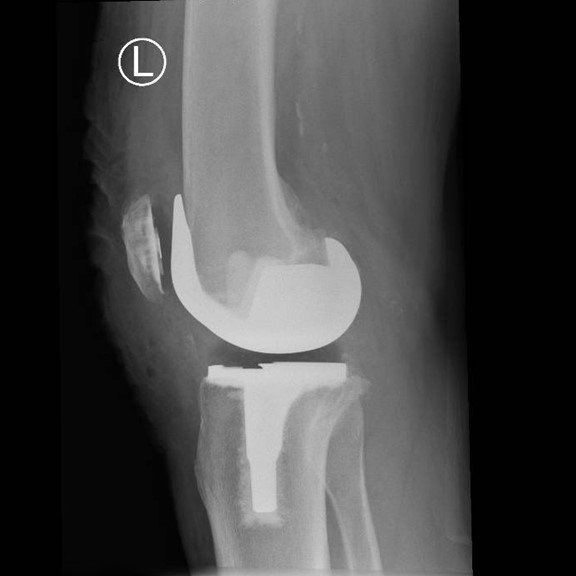
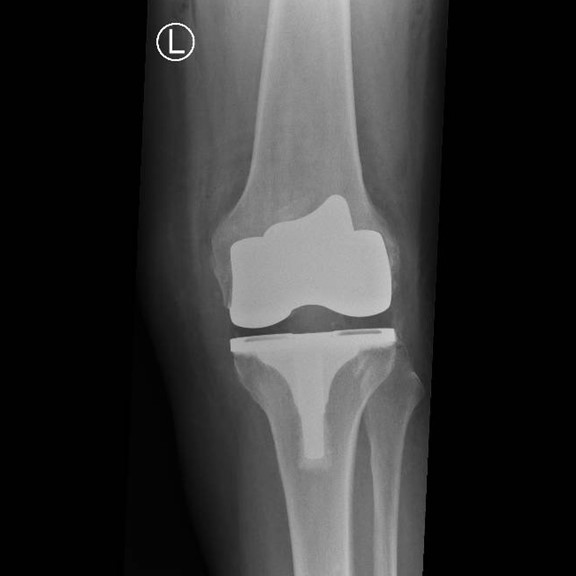
Through a midline incision the surfaces of the bone can be replaced. The femoral component is a smooth metal component of varying sizes, which fits over the end of the femur. The tibial component consists of a metal base plate that sits on top of the tibia and a polyethelene (plastic) insert that fixes onto the tibial component. The patella surface may be replaced if it is worn. The implants are positioned and fixed to the bone using bone cement.
You will be admitted on the day of surgery having not eaten for the preceding 6 hours prior to the operation (nil by mouth). The anaesthetist will talk to you regarding the type of anaesthetic (spinal or general anaesthetic), it is preferable to have a spinal anaesthetic as there are fewer side effects, improved pain control and a speedier rehabilitation whilst in hospital. See FAQ section spinal or general anaesthetic.
After surgery patients generally remain inpatients for 1-3 days. Patients mobilise full weight bearing on the same day of their surgery and generally go home with a stick or crutch for 1-2 weeks. After 4-6 weeks the vast majority of patients will have seen a significant improvement in their knee function.
Risk of surgery
Common
- Bleeding – Bruising following the surgery is common, very occasionally a blood transfusion or iron tablets may be required. Rarely, the bleeding may form a collection within the knee joint which may require a further operation to remove it
- Blood Clots – Deep vein thrombosis (DVT) is a blood clot in a vein. The risk of developing a DVT is greater after surgery (especially lower limb surgery). A DVT can pass in the blood stream and become lodged in the lungs causing a pulmonary embolus (see below). To limit the risk of DVTs forming you will be given stockings to wear on your legs whilst an inpatient and a daily tablet or injection to thin the blood. Moving early after surgery is one of the best ways to prevent blood clots from forming.
- Pain – The knee will be sore after the operation. Pain will improve with time and generally is much improved by the 2 week post-operative mark. Rarely, pain can be a chronic problem.
- Knee Stiffness – This may occur after the operation, especially if the knee is stiff before surgery. If this continues for some time, despite physio input, a manipulation under anaesthesia may be recommended.
- Implant wear and loosening – With modern operating techniques and new implants, knee replacements last in excess of 20 years. In some cases they can fail and this is often as a result of the plastic liner wearing out.
Less Common
- Infection – You will receive antibiotics just before the operation starts and the procedure is performed in a sterile theatre. The wound site may become red, hot and painful. There may be a discharge of pus or fluid. This is usually treated with antibiotics and an operation to washout the joint may be necessary. In rare cases, the implant may be removed and replaced at a later date (revision surgery). The infection can sometimes lead to sepsis (blood infection) and strong antibiotics are required.
Rare
- Pulmonary Embolism – This happens when a blood clot (DVT) breaks off and lodges within the lungs. It can affect breathing and is a serious condition that can be fatal.
- Poor scars – The wound may become red, thickened and painful (keloid scar); this is more common in Afro-Caribbeans.
- Nerve Injuries – Efforts are made to prevent this, however damage to the small nerves of the knee is a risk. This may cause temporary or permanent altered sensation or movement around the knee and lower leg. It is common to have a patch of numbness to the outer aspect of the knee, this generally resolves with time.
- Fracture – Bone may be broken when the new implant is inserted. This may require fixing immediately or at a later date.
- Instability – Rarely the reconstructed joint can be unstable and this can require further surgery.
- Blood vessel injury – Blood vessels at the back of the knee may be damaged, this can require further surgery by the vascular surgeons.
If the arthritis within the knee affects more than one compartment then a total knee replacement may be recommended.
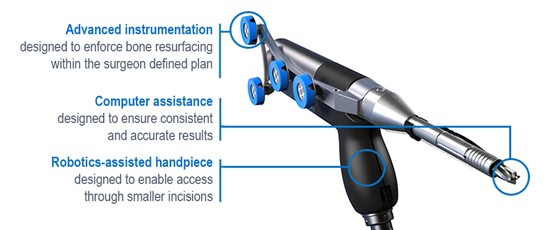

Unlike other robotic systems with the CORI robotic assisted total knee replacement there is no need for further imaging scans such as a CT and therefore radiation exposure is reduced. During a CORI robotic assisted total knee replacement the knee is mapped during surgery using a probe. Tracers can monitor the movement and stability of the knee and an accurate 3D model of the knee is created by the robot. Using this information, the robot can display the optimal sizing and positioning for the implants to enable a balanced, full range of motion. With this level of accuracy, the longevity, function and feel of the knee implant can be improved.
Video provided courtesy of Smith and Nephew
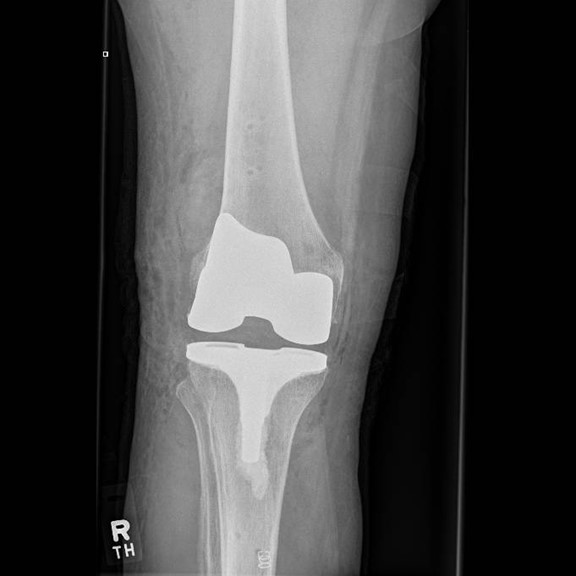
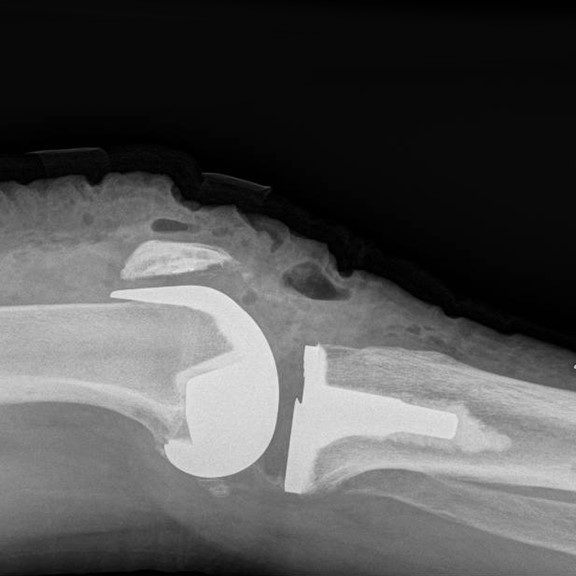
Through a midline incision the surfaces of the bone can be replaced. The femoral component is a smooth metal component of varying sizes, which fits over the end of the femur. The tibial component consists of a metal base plate that sits on top of the tibia and a polyethelene (plastic) insert that fixes onto the tibial component. The patella surface may be replaced if it is worn. The implants are positioned and fixed to the bone using bone cement.
You will be admitted on the day of surgery having not eaten for the preceding 6 hours prior to the operation (nil by mouth). The anaesthetist will talk to you regarding the type of anaesthetic (spinal or general anaesthetic), it is preferable to have a spinal anaesthetic as there are fewer side effects, improved pain control and a speedier rehabilitation whilst in hospital. See FAQ section spinal or general anaesthetic.
After surgery patients generally remain inpatients for 2-4 days. Patients mobilise full weight bearing on the same day of their surgery and generally go home with a stick or crutch for 1-2 weeks. After 4-6 weeks the vast majority of patients will have seen a significant improvement in their knee function.
Risk of Surgery
Common
- Bleeding – Bruising following the surgery is common, very occasionally a blood transfusion or iron tablets may be required. Rarely, the bleeding may form a collection within the knee joint which may require a further operation to remove it.
- Blood Clots – Deep vein thrombosis (DVT) is a blood clot in a vein. The risk of developing a DVT is greater after surgery (especially lower limb surgery). A DVT can pass in the blood stream and become lodged in the lungs causing a pulmonary embolus (see below). To limit the risk of DVTs forming you will be given stockings to wear on your legs whilst an inpatient and a daily tablet or injection to thin the blood. Moving early after surgery is one of the best ways to prevent blood clots from forming.
- Pain – The knee will be sore after the operation. Pain will improve with time and generally is much improved by the 2 week post-operative mark. Rarely, pain can be a chronic problem.
- Knee Stiffness – This may occur after the operation, especially if the knee is stiff before surgery. If this continues for some time, despite physio input, a manipulation under anaesthesia may be recommended.
- Implant wear and loosening – With modern operating techniques and new implants, knee replacements last in excess of 20 years. In some cases they can fail and this is often as a result of the plastic liner wearing out.
Less Common
- Infection – You will receive antibiotics just before the operation starts and the procedure is performed in a sterile theatre. The wound site may become red, hot and painful. There may be a discharge of pus or fluid. This is usually treated with antibiotics and an operation to washout the joint may be necessary. In rare cases, the implant may be removed and replaced at a later date (revision surgery). The infection can sometimes lead to sepsis (blood infection) and strong antibiotics are required.
Rare
- Pulmonary Embolism – This happens when a blood clot (DVT) breaks off and lodges within the lungs. It can affect breathing and is a serious condition that can be fatal.
- Poor scars – The wound may become red, thickened and painful (keloid scar); this is more common in Afro-Caribbeans.
- Nerve Injuries – Efforts are made to prevent this, however damage to the small nerves of the knee is a risk. This may cause temporary or permanent altered sensation or movement around the knee and lower leg. It is common to have a patch of numbness to the outer aspect of the knee, this generally resolves with time.
- Fracture – Bone may be broken when the new implant is inserted. This may require fixing immediately or at a later date.
- Instability – Rarely the reconstructed joint can be unstable and this can require further surgery.
- Blood vessel injury – Blood vessels at the back of the knee may be damaged, this can require further surgery by the vascular surgeons.

